Hives, also known as urticaria, are an outbreak of red, swollen bumps that appear suddenly on the skin. They are a result of your body’s reaction to an allergen or situation. Almost 20 percent of people will experience hives at some time in their life.
Causes
When you come into contact with certain foods, insect stings, sunlight or medications that you are allergic to, your body will release a chemical called histamine. In response to histamine, your skin can become itchy with swollen red welts.
There are two types of hives: acute and chronic. Acute hives last less than six weeks and are usually caused by certain foods (the most common are nuts, chocolate, fish, tomatoes, eggs, fresh berries, milk and certain food additives or preservatives), medications, insect stings or infections.
Chronic hives last for more than six weeks. The cause of this type of hives is more difficult to determine. Often, they appear because of thyroid disease, hepatitis, infection, autoimmunity or cancer. For some, the cause is never determined.
Pollen, pet dander, latex and physical stimuli, such as pressure, cold, heat, exercise or sun exposure are also common hives triggers.
Symptoms
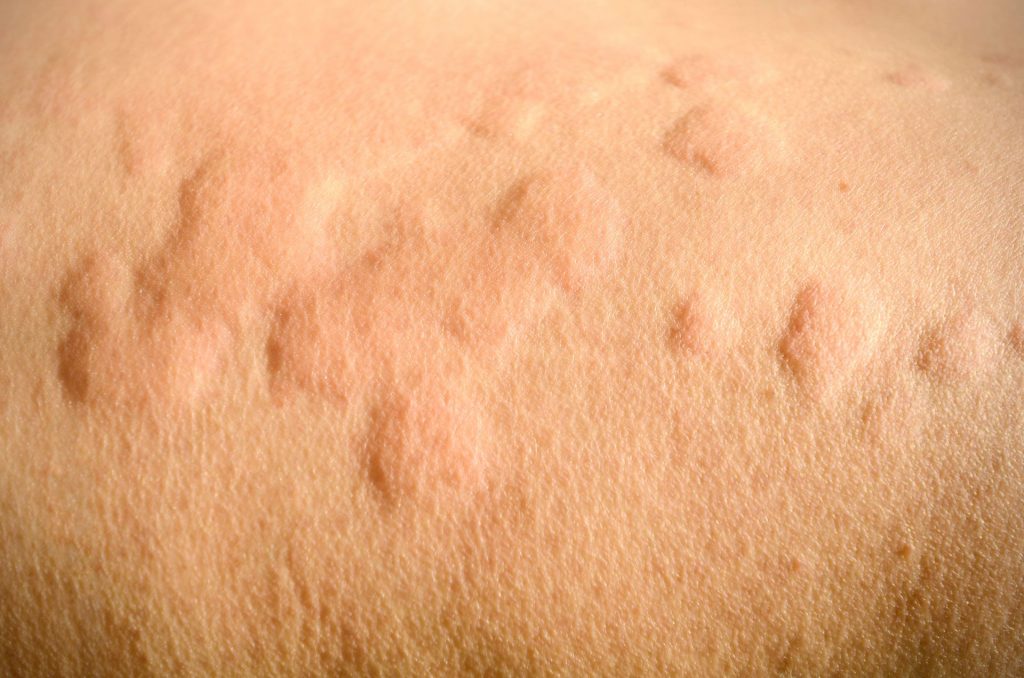
Hives often resemble a bug bite. But unlike a bite, they can appear anywhere on the body, change shape, move around, disappear and reappear over short periods of time. The bumps (also called wheals) will be red or skin colored with clear edges. When pressed, the center of the hive will turn white; this is called blanching.
Angioedema is a condition commonly mistaken for urticaria. Swelling takes place below the surface of the skin instead of on the surface. An allergic reaction, medications or an enzyme deficiency can cause angioedema to appear. Common symptoms are swelling of the eyes or mouth, swelling of the hands, feet or throat, difficulty breathing, stomach cramps and swelling of the lining of the eyes.
Treatment
The first thing your doctor will do is try to determine the cause of your hives. While some triggers are easy to identify, others may require a process of elimination.
Your doctor will review you and your family’s medical history as well as ask questions about your exposure to potential allergens like pets or medication.
Next, your doctor will complete a skin prick test and/or a blood test to confirm if you are allergic to any foods or medications. Avoidance of a particular food or drug will be recommended if these tests come back positive.
If your hives are determined to have a physical cause, such as exposure to heat, cold or pressure, your doctor will recommend the following:
- Avoid tight clothing.
- Avoid exposure to cold air. If you must go out in the cold, wear warm clothing and use a scarf to cover your nose and mouth.
- Avoid sun exposure by wearing protective clothing and sunblock.
Antihistamines, which are available either over-the-counter or by prescription, are typically recommended for the treatment of hives. These drugs are effective for long-term use and have few side effects. For those with severe episodes of urticaria, a corticosteroid medication or immune modulator can be used to reduce the symptoms.
If you have trouble breathing or have swelling of your lips or tongue, your doctor may prescribe an epinephrine auto-injector for you to carry with you at all times. These symptoms may lead to anaphylaxis, a potentially fatal allergic reaction that can only be treated with an auto-injector.
